You've probably heard the term CBT thrown around - by your GP, a friend who's been in therapy, or maybe on a mental health app. But what does it actually mean? What happens in a CBT session? And is it just being told to "think positive"?
It's none of that last one. CBT (Cognitive Behavioural Therapy) is one of the most extensively researched psychological treatments in the world, and it's a lot more practical, grounded, and empowering than most people expect. Whether you're working with a therapist, exploring self-help tools, or just trying to understand your own mind a little better, this guide is your starting point.
CBT stands for Cognitive Behavioural Therapy - and those three words each matter. Cognitive refers to your thoughts and the way you interpret the world. Behavioural refers to the things you do (or avoid doing) in response. Therapy is the structured process of examining and shifting both. Put it together and you get an approach that helps you understand the connection between what you think, how you feel, and what you do - and then gently, practically, helps you change the patterns that are keeping you stuck.
It was developed in the 1960s by psychiatrist Aaron Beck, who noticed that his patients' emotional difficulties were closely linked to their patterns of thought - particularly automatic, negative interpretations of events.
His insight was simple but radical: if the way you think shapes the way you feel, then changing the way you think can change the way you feel. Decades of research have backed this up, and CBT is now one of the most widely used evidence-based therapies in the world.
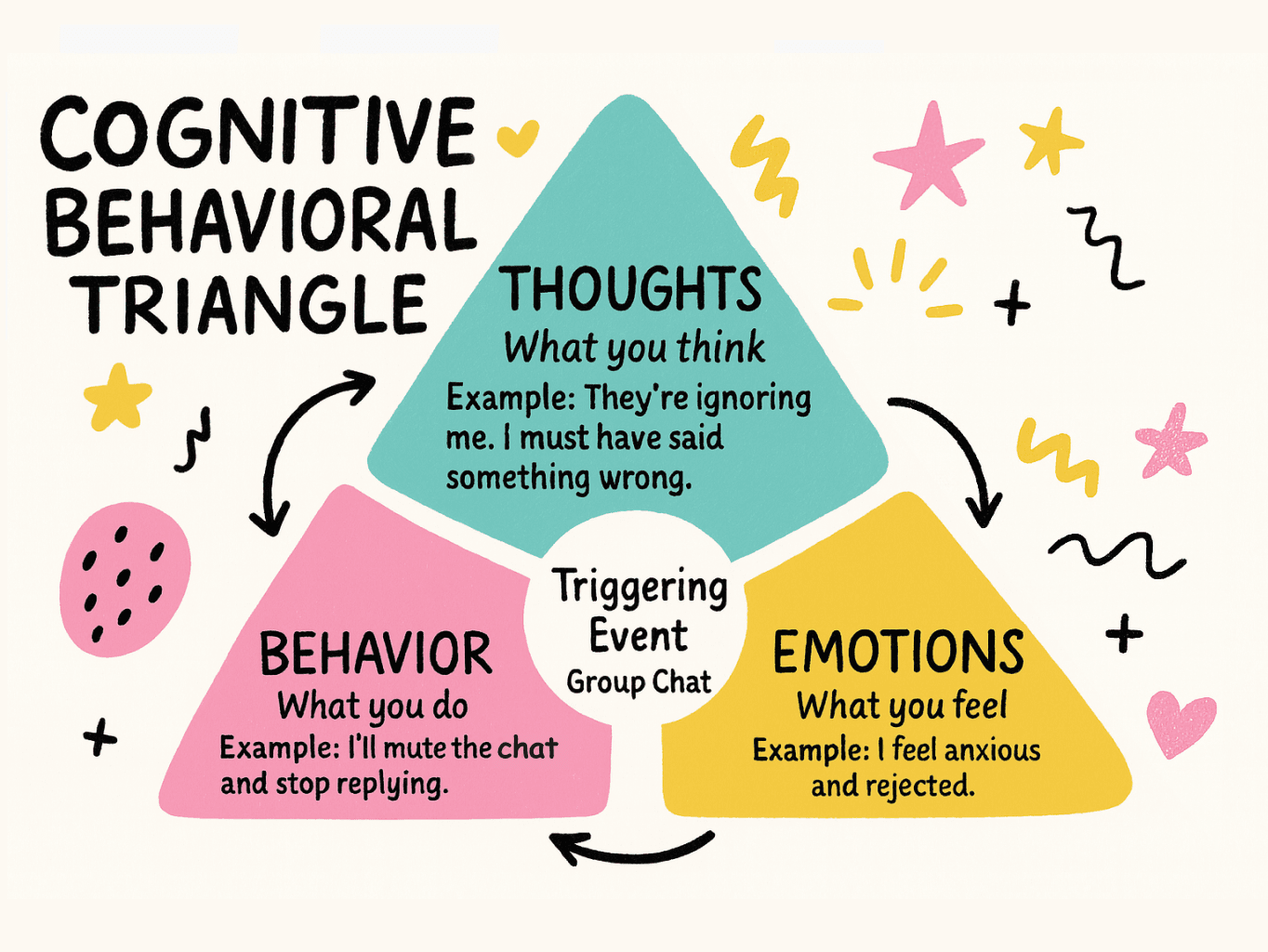
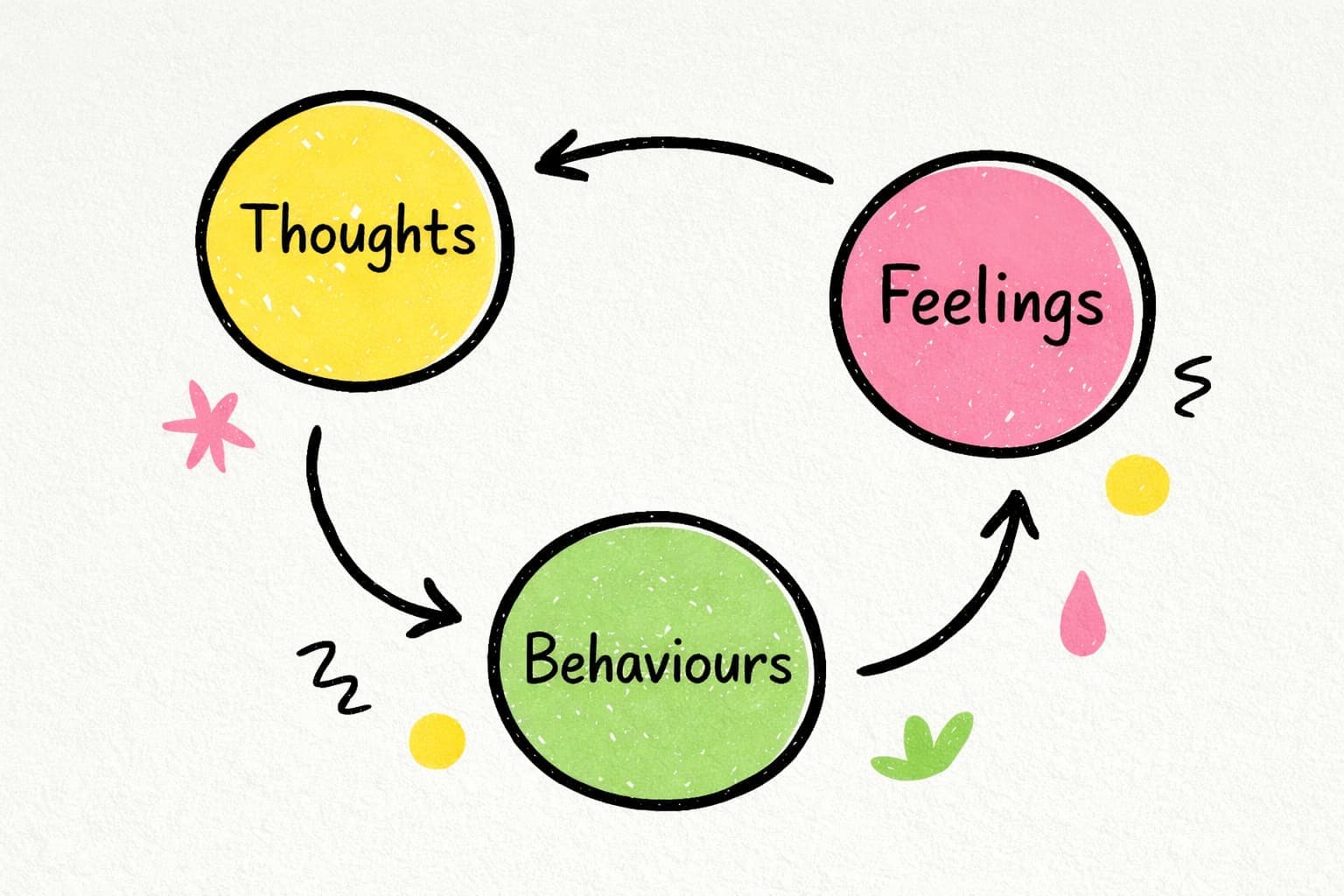
At the heart of CBT is something called the cognitive triangle — the idea that thoughts, feelings, and behaviours constantly influence each other in a loop. It works like this:
🧠 A thought arises - "I said something stupid in that meeting."
😔 That thought creates a feeling - shame, anxiety, dread.
🚪 That feeling drives a behaviour - you avoid speaking up in the next meeting.
🔁 That behaviour reinforces the thought - "See, I'm better off staying quiet. I always mess things up."
And the cycle continues. What CBT does is interrupt that loop - by helping you notice the original thought, question whether it's actually accurate, and try different responses that break the cycle rather than deepen it.
As Cleveland Clinic explains, CBT focuses on identifying and challenging unhelpful thought patterns and modifying the behaviours that maintain them (clevelandclinic.org).
Crucially, CBT doesn't try to replace all negative thoughts with positive ones. That would be unrealistic and, frankly, patronising. The goal is accurate and helpful thinking - seeing situations more clearly, rather than through a lens of fear, self-criticism, or catastrophe.
Yes - and the evidence base is substantial. A landmark meta-review published in Psychological Medicine, summarising 494 reviews covering more than 221,000 participants, found that CBT produced consistent, meaningful benefits across a wide range of mental and physical health conditions (Cambridge Core, 2021).
A separate large-scale naturalistic study of over 6,600 patients found meaningful symptom improvement in the vast majority of people who completed CBT treatment, with fewer than 2% reporting worsening (ScienceDirect, 2025).
Crucially, the gains from CBT tend to last. Unlike medication, which manages symptoms while you take it, CBT teaches you skills - ways of thinking and responding that stay with you long after therapy ends.
The British Association for Behavioural and Cognitive Psychotherapies (BABCP) describes it as designed specifically around what works, based on decades of scientific research (babcp.com).
CBT is remarkably versatile. It was originally developed for depression, and remains one of the most effective treatments for it. But over the decades, it's been adapted and proven effective for a wide range of conditions and challenges, including:
😰 Anxiety disorders - generalised anxiety, social anxiety, panic disorder, health anxiety
😔 Depression - including chronic and recurrent depression
🔁 OCD - Obsessive Compulsive Disorder and related conditions
😨 PTSD - Post-Traumatic Stress Disorder and trauma responses
😴 Insomnia - CBT for insomnia (CBT-I) is now the first-line recommended treatment
🍽️ Eating disorders - including bulimia and binge eating disorder
😤 Anger and stress - including workplace stress and burnout
💊 Chronic pain and fatigue - helping people relate differently to physical symptoms
Beyond clinical conditions, CBT is also widely used to support people through difficult life events - relationship challenges, work stress, grief, low self-esteem, and the kind of everyday anxiety that never quite tips into a diagnosis but still makes life harder than it needs to be.

CBT isn't just talking about your problems — it involves specific, practical tools and exercises, many of which you do between sessions as homework. The most common include:
📝 Thought records - one of CBT's best-known tools, a thought record helps you spot automatic negative thoughts, examine the evidence for and against them, and arrive at a more balanced view. If you want to try one right now, Offload's Thought Record tool walks you through every step
🔬 Behavioural experiments - rather than just challenging a thought on paper, you test it in real life. "I believe people will judge me if I speak up. Let me try it once and see what actually happens." Check out Offload’s Behavioural experiment tool.
🪜 Exposure and response prevention (ERP) - gradually facing feared situations or objects rather than avoiding them, used particularly in anxiety and OCD. Check out Offload’s mini course on ERP.
🎯 Behavioural activation — scheduling small, meaningful activities to break the cycle of low mood and withdrawal, often used in depression. Check out Offload’s mini course on Behavioural activation.
🌀 Grounding and relaxation techniques — tools to manage acute anxiety and bring you back to the present moment. See the relaxation tools library.
What links all of these is the same underlying principle: your thoughts and behaviours are learnable skills, and what can be learned can be unlearned and relearned. If you're curious about how the most common unhelpful thinking patterns work, our guide to cognitive distortions breaks them down one by one.
CBT sessions are structured and collaborative - quite different from the "lie on a couch and talk about your childhood" image some people have of therapy. A typical session might involve reviewing how the previous week went, working through a specific situation that caused distress using one of the tools above, identifying patterns, setting a between-session task, and checking in on progress toward a goal.
Most CBT courses run for somewhere between 6 and 20 sessions, depending on what you're working on. Sessions are usually weekly and last around 50 minutes. One of CBT's defining features is that it's explicitly time-limited and goal-focused - you're working toward something concrete, not just processing indefinitely. That said, the skills you develop during a CBT course are designed to stick: the long-term aim is for you to become your own therapist, able to apply the tools independently whenever you need them.
Between sessions, the work continues. Tools like mood tracking, thought records, and activity logs help build self-awareness and give your therapist real insight into how you're actually doing day to day. Offload is designed specifically to make this between-session practice easier - so the work doesn't stop when you close the therapy room door
CBT is highly effective for a lot of people, but it's worth being honest: it's not a magic fix, and it does require active participation. You'll get the most out of it if you're willing to engage with the exercises between sessions, sit with some discomfort as you challenge longstanding patterns, and keep going even when early sessions feel hard.
Some people find that other approaches — like ACT (Acceptance and Commitment Therapy) or DBT (Dialectical Behaviour Therapy) — suit them better, or that a combination works best. Both ACT and DBT share roots with CBT but take slightly different angles. A good therapist will work with you to find the approach that fits.
What CBT does offer almost everyone, regardless of whether you're in formal therapy, is a set of tools that are practical, evidence-based, and learnable. You don't need a diagnosis to benefit from understanding your own thinking patterns better.

One of the most empowering things about CBT is that it doesn't end when therapy does. The thought record you learn in week three, the behavioural experiment you try in week seven, the way you start to notice your own thinking patterns — all of that stays with you. Research consistently shows that people who actively practise CBT skills between sessions have better outcomes and are more resilient to relapse in the long run.
That's exactly why Offload exists. Our library of 200+ interactive, evidence-based tools — including thought records, mood trackers, journals, and psychoeducation — is built to make those between-session skills feel accessible, approachable, and genuinely useful rather than like homework you'll never get round to. Whether you're a client assigned tools by your therapist, or someone exploring independently, these are the same techniques that decades of research have shown to work.
Ready to explore? Take a look at all the tools available in Offload
Cognitive Behavioural Therapy is a structured, evidence-based psychological treatment built on the insight that how we think shapes how we feel and behave. Developed in the 1960s and refined through decades of research, it's now the most widely studied form of therapy in the world, with proven effectiveness for anxiety, depression, OCD, PTSD, and much more. CBT works by teaching practical skills — thought records, behavioural experiments, exposure techniques — that interrupt unhelpful cycles and build lasting resilience. Unlike many treatments, it's explicitly designed to give you tools you keep using long after the sessions are done.
Related Articles